
by Demetria | Apr 30, 2025 | Uncategorized
Essential Postpartum Tips for Doulas: Empowering New Parents on Their Journey Welcoming a new life into the world is a profoundly beautiful journey, but it also comes with its own unique challenges, especially during the postpartum period. As doulas, we play a crucial...
by Demetria | Apr 16, 2025 | Uncategorized
🍼 10 Powerful Reasons to Hire a Doula Discover how doulas can transform the birth experience—for you, your baby, and your whole family. If you’re exploring the reasons to hire a doula, you’re already on the path toward a more supported and empowering birth. Doulas...

by Demetria | Feb 26, 2025 | Uncategorized
Become a Breastfeeding Educator and Make a Difference Becoming a Breastfeeding Educator is a rewarding and impactful career choice, offering the opportunity to make a real difference in the lives of parents, babies, and communities. Here are some compelling reasons...

by Demetria | Feb 26, 2025 | doula, postpartum doula
What will I learn? Check out the skills and competencies that Breastfeeding Educator Certification can offer you. Core Educational Components (200 Hours) I. Lactation Science & Physiology (60 Hours) Breast anatomy and physiology Hormonal regulation of lactation...
by Demetria | Nov 13, 2024 | business, doula, postpartum doula
Unlock Your Career Potential with MYCAA Funding at Birth Arts International Are you a military spouse looking to build a rewarding career in birth work? Birth Arts International proudly supports military families by offering eligible programs that qualify for the My...
by Demetria | Nov 6, 2024 | business, doula, postpartum doula
Why You Should Become a Birth Arts International Doula Are you passionate about empowering families through one of life’s most significant moments? Becoming a doula could be the perfect path for you. At Birth Arts International, we train compassionate, skilled doulas...
by Demetria | Oct 30, 2024 | doula, postpartum doula
The Role of a Doula: How Birth Support Shapes Unique Family Experiences The role of a doula is unique and crucial in creating positive birth experiences.Childbirth is a significant life event, and having the proper support can make a huge difference. At Birth Arts...
by Demetria | Oct 27, 2024 | doula, postpartum doula
What is a Doula? Understanding the Role and Benefits When preparing for childbirth, many parents picture doctors or midwives leading the way. But there’s another vital support figure—a doula. At Birth Arts International, we believe in compassionate, hands-on...
by Demetria | Oct 16, 2024 | business, doula, postpartum doula
Already Certified? Are you already certified through Birth Arts International? Do you need a copy of your certificate sent? Please use this option. Can’t find your certificate and need another copy? Use this option. Do you need to change the name on your...
by Demetria | Sep 24, 2024 | doula, postpartum doula
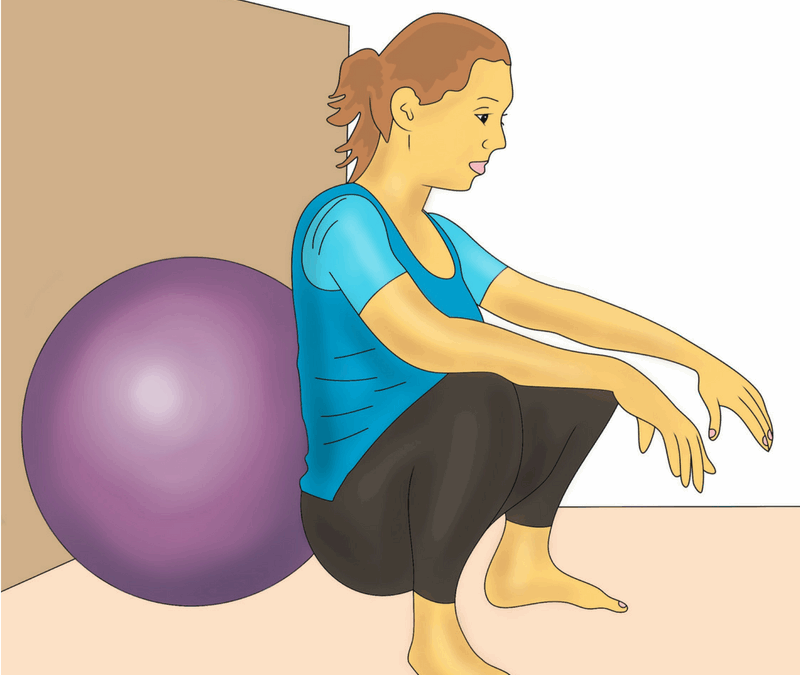
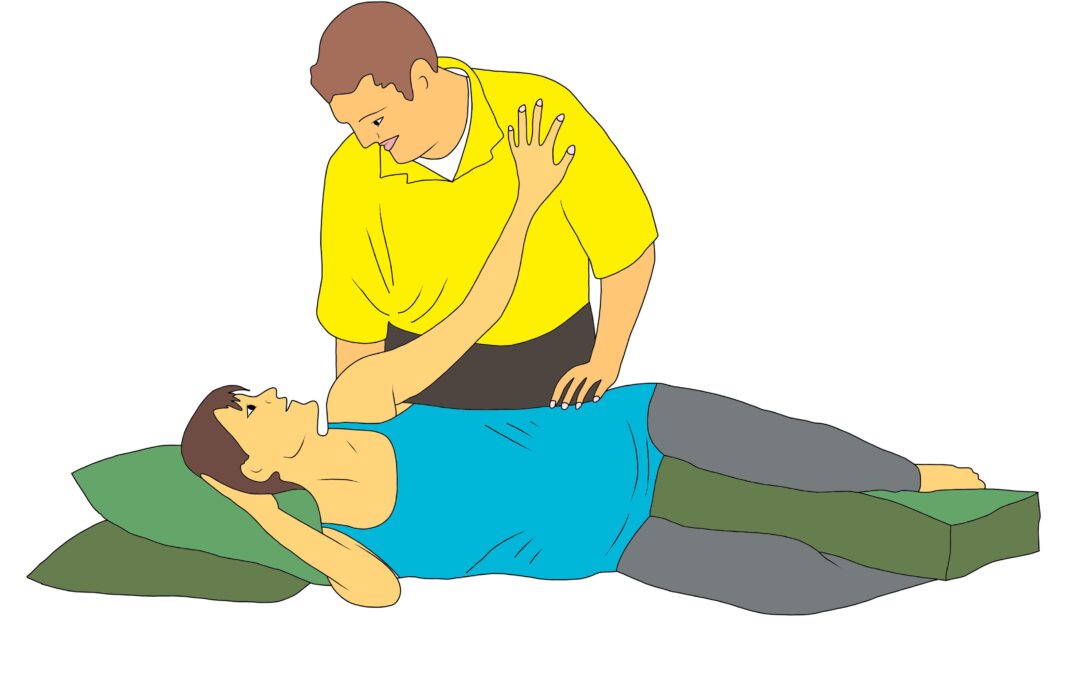
Best Birth Positions for Doulas to Support Laboring Clients As a doula, understanding various birth positions and their benefits can significantly enhance your ability to support a birthing person. Different positions not only help manage pain and facilitate the...






